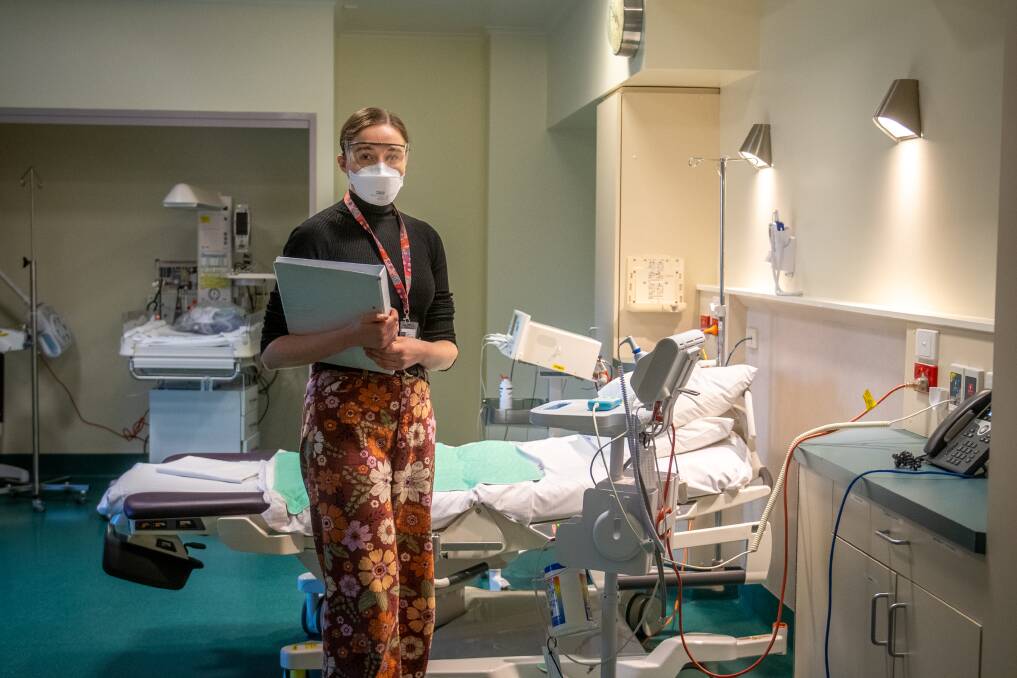
About 1600 babies are born at the Launceston General Hospital each year.
Subscribe now for unlimited access.
or signup to continue reading
For a regional hospital like the LGH, that number of births places an enormous workload on the staff whose job it is to support mothers and families through the pregnancy process.
The strain can also be acutely felt by the parents, particularly those young or first-time mothers experiencing their first taste of parenthood.
To manage the needs of the patients the Launceston General Hospital established the Midwifery Group Practice in march 2014, an expert team of midwives who provide end-to-end care for prospective parents.
Midwifery group practice, sometimes called caseload midwifery, is a patient-centric model of care in which a pregnant woman is looked after by the same small group of midwives during their pregnancy, during childbirth and in the weeks after a baby is born.
The patient-first-focus allows for a more individual and tailored approach to care in which the patients and midwives can develop a relationship of trust that provides the mother with 24-hour access to their own midwives.
UK-born Isobel Holmes is a midwife at the Launceston General Hospital who works in the Midwifery Group Practice unit.
A strong advocate of the benefits that group practice provides, Ms Holmes describes the service as the "gold standard" of care for expectant mothers.
"We look after women all the way through their pregnancy in a small group as midwives, there are usually two or three midwives that the women get to know throughout their pregnancy," she said.
At the heart of the program is the principle of continuity of care, a method of patient care that promotes the development of a strong relationship between the patient and their clinical team.
However, midwifery group practice takes the concept one step further.
"They have our contact numbers, '' Ms Holmes said.
"They can call us with questions and concerns, and we just focus on building that relationship throughout the pregnancy, getting to know their birth preferences and their family - we're there to support them."
Working in teams of two and three, a midwife is always on call to provide support for an expectant mother - day or night - and when the time comes, one of the patient's dedicated midwives will be present for the birth.
Ms Holmes says one of the main goals, other than the continuity of care, was keeping patients out of hospital for as much of their pregnancy as possible.
"The philosophy of midwifery is that we're caring for women who are generally well, it's a normal process having a baby so keeping them out of the hospital is ideal," she said.
"We get called in for the birth and we're there when they have their baby, then it's an early discharge program.
"We aim to discharge them within four to six hours after the birth if there have been no complications, and then we do community-based home visits for the rest of the postnatal care."
While keeping pregnant women out of hospital - thus reducing overall pressure on the hospital - is one of the benefits of the program, group practice also has health benefits for the mother and their baby.
Increased rates of breastfeeding and fewer complications at birth have been found in mothers who go through the program - outcomes Ms Holmes attributes to the group practice model.
Building that relationship and having a midwife - the research has consistently shown how it can improve outcomes such as reducing premature birth or reducing caesarean section rates and less time in labour - there's just a whole host of benefits for women
- Isobel Holmes
"Building that relationship and having a midwife - the research has consistently shown how it can improve outcomes such as reducing premature birth or reducing caesarean section rates and less time in labour - there's just a whole host of benefits for women," she said.
"Then for midwives, it's also great job satisfaction as well, getting to know the women and seeing them through that journey."
Chloe McCreary is a mother of four who went through the group practice for her third and fourth births.
She said while the midwives she had for her first two births were excellent, the personal connection she formed with her midwifery team during her later births gave her more support.
"My 2016 birth, I had a few [complications] towards the end and I was classified as high risk," she said. "I had low amniotic fluid and my baby was in breech, that means coming bum or feet first rather than head first, so I ended up having an elective caesarean section with her."
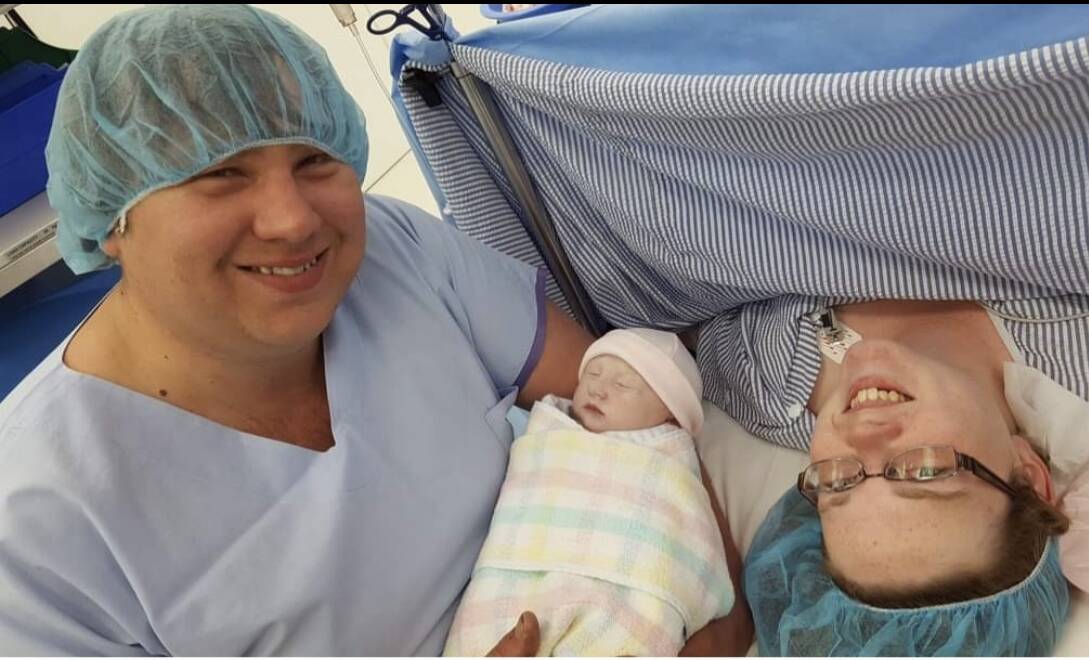
While the caesarean was not part of Ms McCreary's birth plan, she said the voluntary procedure was the best method for her baby at the time, but not something she wanted to repeat for her fourth child.
"In 2020 the birth of our son was what they call a VBAC, so a vaginal birth after c-section, which I was very pleased to attempt and be allowed to attempt," she said.
"Sometimes, once you've had the c-section you need one every other time, so I was very happy that Janet was there to stand up for me when the doctors were a bit apprehensive."
She said her recovery from the VABC was much shorter than what she experienced after her caesarean.
"Recovery was quite quick in comparison to my C-section," she said.
"My son was born quite late in the day, so I did end up staying overnight with him, but I went home the next morning.
"Janet did give me the option to go home that night, but having three kids at home, I was more than happy to stay overnight."
While group practice aims to have the same midwives see each mother through their individual pregnancies, Ms McCreary was fortunate enough to have the same midwife for the two of her births that went through the unit.
She said she was so pleased with the personal service she received from her midwife Janet Russell that she nominated her for the Launceston General Hospital's Daisy award - an award that recognises the extraordinary work of nurses and midwives at the hospital - and an award that Ms Russell won.

At 27, Ms Holmes is still in the career-building phase of her professional life, despite displaying an encyclopaedic knowledge of the midwifery practice - a knowledge clearly matched by her passion for the profession.
She said a family history of midwifery and exposure to childbirth at a formative age was the catalyst for her to take up the profession.
"My grandmother was a midwife in York in the 1950s and 60s, and so her stories were quite inspiring, then my mum had a baby when I was 17 and that was really what motivated me to study midwifery," she said.
Originally from York in the UK, Ms Holmes' journey to the Launceston General Hospital has been anything but conventional.
After completing a direct entry degree in midwifery at the University of the West of England in Bristol, Ms Holmes took a sabbatical, travelling to Tasmania where she worked as an au pair for four months, before extending her stay and working as a berry picker.
Falling in love with Tasmania and all it has to offer, Ms Holmes bought a house and took a job at the LGH.
As part of her progression through the profession, Ms Holmes has begun studying for her masters of primary maternity care through Griffith University.
Along with another midwife in her unit, Geraldine Beauben, Ms Holmes's commitment to the profession was recently recognized by the Department of Health who awarded both a scholarship under the inaugural Tasmanian Nursing and Midwifery Scholarship.
Each scholarship is sponsored by the office of the chief nurse and midwifery officer and is valued at $2000, intended to support Tasmanian Health Service nurses and midwives who are undertaking career progressing study.
With a full workload, including shift work and being on call, Ms Holmes said receiving the award would lessen the burden of working and studying at the same time.
"It's quite hard work, studying and working at the same time, so to know that we have that backing and support behind us it's been really great," she said.
"It's really motivating, that we're supported to do the study.
Karen Monroe is the Midwifery Group Practice coordinator at the Launceston General Hospital and said for not one but two midwives to receive the scholarship was a great outcome for the unit and the hospital.
"I encourage midwives to do further education, It's a financial boon for them," she said.
"I've actually got three of our MGP midwives studying their clinical masters of midwifery.
"Whatever helps the midwives continue working while they're studying is absolutely a boon for me, and I'm very pro-education - you never stop learning."
Ms Monroe said while group practice had become increasingly popular with expectant Northern mothers, limited resources meant the hospital was unable to offer the service to all - something she hoped would change in the future.
"We're quite a popular program," she said
"I've just had a text message from a repeat woman saying I'm pregnant again... can you save your spot?
"I do run a waitlist and we do have criteria. We started off as a low-risk model, but now we do take high-risk women."
Ms Monroe said she hoped coming out of COVID the hospital would be in a better position to grow the midwifery program.
"I am continually asking for more midwives, but at the moment we've got a chronic shortage of midwives and I think COVID has really heightened that," she said.
"We are super keen to expand, I've got waitlists with at least 20 women that generally are wanting to get onto the program.
"I'll ring women up at 34-35 weeks and say, "I've actually got a spot, do you want to come across" and often they will.
"We would love to expand... definitely."

Our journalists work hard to provide local, up-to-date news to the community. This is how you can continue to access our trusted content:
- Bookmark www.examiner.com.au
- Make sure you are signed up for our breaking and regular headlines newsletters
- Follow us on Twitter: @examineronline
- Follow us on Instagram: @examineronline
- Follow us on Google News: The Examiner














