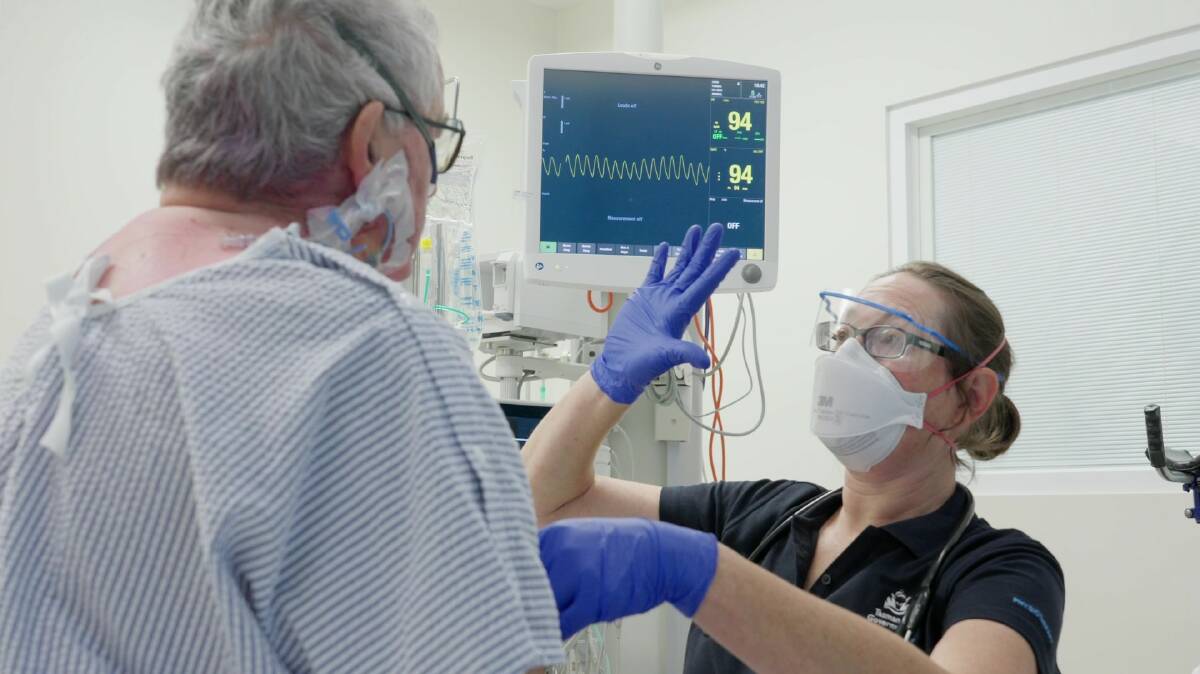
Pneumonia is one of the top five causes of death in Tasmania and one of the most common complications for people following major surgery, however, a world-first study by a Launceston clinician is uncovering new treatments that could curb infections.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
For the past decade Launceston General Hospital physiotherapist Dr Ianthe Boden has been researching ways to prevent pneumonia and improve patient recovery after major surgery, with her latest study showing promise after recently being published in the prestigious Journal of Trauma and Acute Care Surgery.
An acute respiratory infection that affects the lungs by filling sacs called alveoli with fluid instead of air, pneumonia can cause pain, inflammation and difficulty breathing in patients, and in extreme cases death.
"We know pneumonia is the second most common complication after this type of [abdominal] surgery," Dr Boden said.
"It's the leading cause of organ failure and the fourth leading cause of death, so it's the worst of both worlds. It happens really frequently and has catastrophic effects."
The published study called ICEAGE incidence of complications following emergency abdominal surgery - get exercising was funded with $80,000 from the Clifford Craig Foundation.
After noticing a gap in the literature on preventative measures for people coming out of emergency abdominal surgery, Dr Boden undertook a new study to address the issues of postoperative pneumonia.
"When I looked at what had been published in the scientific literature, I found nothing... a big glaring abyss of nothingness had been published related to this problem, so I thought we have to fix that.," she said.
"My question was what are we doing about it, from a hospital perspective, how do we help our patients to first of all not get pneumonia and secondly, how can we help them get back to normal a lot faster."
In 2015, Dr Boden commenced a randomised control trial with the pilot phase finding early intensive physical therapy made up of coached breathing exercises and 30 minutes of assisted physical activity delivered daily in the first five days surgery was safe and feasible.
She said the initial research was essential to ensure increasing the rate of physical activity in postoperative patients could be undertaken safely.
"The first paper is all about safety," she said.
"If it wasn't safe, we couldn't have gone on to the bigger trial... you have to answer that question first and the final trial will answer the question about pneumonia and whether or not patients get better quicker," she said.
After the pilot found the study was safe to administer increased physical therapy, the study moved to a multi-centre trial phase, which provided world-first evidence that early intervention had the potential to prevent pneumonia and improve recovery after emergency abdominal surgery.
READ MORE: Firefighters defiant, pay clash smoulders on
While a paper on the final results of the trial is not yet complete, Dr Boden said the preliminary results were already proving "very positive".
"The very sneak-peak result is that it works really, really well," she said.
"There's a 60 per cent reduction in pneumonia rates and that's big, there's nothing else that's even come close to reducing pneumonia like that."
As a world-first study, Dr Boden's ICEAGE has been celebrated globally with the preliminary findings winning best paper at the 2018 Royal Australasian College of Surgeons Annual Trauma Symposium.
A year later results were presented at the 2019 World Congress of Physical Therapy in Geneva, Switzerland where the study was named best clinical trial.
Our journalists work hard to provide local, up-to-date news to the community. This is how you can continue to access our trusted content:



