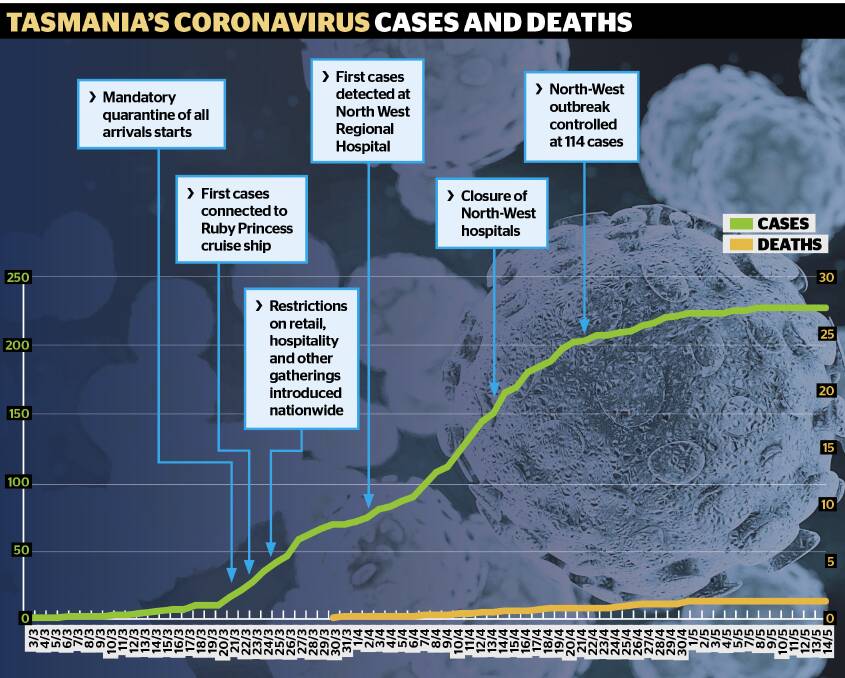
It seems an age ago that Launceston and Hobart were first confronted with the grim reality of the coronavirus, having watched from afar as China, Iran and Italy were overrun with mass casualties.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
As far as public health authorities can tell, the virus first arrived in Tasmania on February 26, carried by a hospitality worker who travelled from Nepal via Singapore. It was not publicly confirmed until March 7, and the man, in his 20s, had visited night spots and worked shifts at a busy Hobart hotel.
It came a few days after a man arrived in Launceston from Iran with the virus. He was ordered to quarantine, but on his way home he made a quick stop at Woolworths on Wellington Street.

The announcements seemed like moments frozen in time. Was the virus already moving from person to person undetected in Hobart? Had droplets been left on a checkout in Launceston for the next customer? The sense of unknowing affected every Tasmanian.
Yet it appears almost certain that these cases stopped at the source. Contact tracing did not pick up any other cases from the two men.
Was this simply good fortune? Judging by the subsequent experience across the world, the virus seems more transmissible than we knew at the time. University of Tasmania senior lecturer in ecology and epidemiology Scott Carver is reluctant to say we were "lucky".
"The vast majority of transmissions happen between close personal contacts and has continued to happen that way, but you can get transmission through other mechanisms such as shared surfaces. Possibly we've been fortunate that a couple of these early situations appear to have not led to community transmission," he said.
"The response was quite swift and in advance of community transmission."
With the state's borders still completely open, the third case carried the virus from South America, the fourth from the Philippines and the fifth from North America before further cases were confirmed as close contacts of these returned travellers.

On March 18, three more cases were found in the South having arrived from overseas. Three days later, Tasmania saw its biggest jump with five new cases, all returned travellers - including the state's first encounter with the notorious Ruby Princess cruise ship debacle, which disembarked in Sydney on March 19.
It was at this time, March 20, that Tasmania introduced the toughest border restrictions in Australia, making use of its island status to force all arrivals into 14 days quarantine in response to growing community concern.
This measure was adopted by other states not long after, recognising the risk of having people walk unchecked through airport security and into the community, like the two mainlanders who visited 21 Tasmanian tourism hotspots between March 12 and 23 only to later test positive to the coronavirus. Fortunately, only one tourism operator went on to test positive as a result.
The travel restrictions helped to catch Ruby Princess passengers just in time. Public Health Services urgently traced international arrivals, but the sheer volume of positive cases linked to cruise ships caught everyone by surprise.

From March 21 to 27, 48 new cases were detected. The vast majority were from cruise ships, with Ovation of the Seas now also a source of infection. In the midst of this surge in infections, nationwide restrictions were introduced on retail, hospitality and all gatherings, although each state chose its own path.
With so many cases being picked up, fears of community transmission were once again ignited. The confirmation that a staff member at Mersey Community Hospital had contracted the virus highlighted the risks faced by our frontline healthcare workers.
It also became inevitable that Tasmanians would die as a result of the coronavirus, with many of the new cases elderly.
"I have been saying for weeks that this is serious, that people will die and unfortunately Tasmania now has its first death," Premier Peter Gutwein said at the time. "All Tasmanians need to accept and understand that this is not a game, this is serious, people's lives are at risk."
In the meantime, the coronavirus was unknowingly spreading among staff at the North West Regional Hospital, originating in two elderly patients who contracted the virus on the Ruby Princess.

While the rate of virus detections from interstate and overseas slowed to a stop, the NWRH cluster quickly caused another surge - and it proved to be deadly. The first two cases among staff were confirmed on April 2, with a further 11 experiencing symptoms.
Over the coming weeks, the hospital outbreak became the focus of public health efforts. After April 6, almost all coronavirus cases in the state were linked to the hospital cluster, resulting in the drastic step of closing the NWRH and North West Private Hospital on April 13 to undergo a deep clean.
The North-West situation became the largest source of new cases anywhere in Australia at various stages in April, and will be used as an example of how to avoid hospital virus outbreaks for years to come. It resulted in 114 cases and 11 deaths by April 21, when it was finally under control, although a small number of cases continued to be detected among close contacts into May.
An interim report into the outbreak found staff had continued to work while symptomatic, spreading the coronavirus during meetings. There were also shortcomings in infectious disease practices.

The state's focus has now turned to widespread community testing, with a doctor's referral easily available. For a week from May 7, there were no new cases. But public health director Mark Veitch said it would be many months before Tasmania could be declared coronavirus-free.
Dr Carver said putting science at the centre of decision-making had allowed Tasmania, and Australia more widely, to avoid the worst of the pandemic.
"Tasmania has achieved a very high level of control quite successfully with a virus that is exceptionally challenging to control. There is a good chance that we may achieve viral eradication," he said.
"Tasmania is right up there with New Zealand in terms of successful disease control."
But the job is only half done, with new dangers emerging as economies reopen and domestic travel restarts.
"The more testing we do, the more likely it is that we pick up those asymptomatic cases," Dr Carver said. "I don't think anybody wants to categorically say there are no cases floating around in Tasmania."


