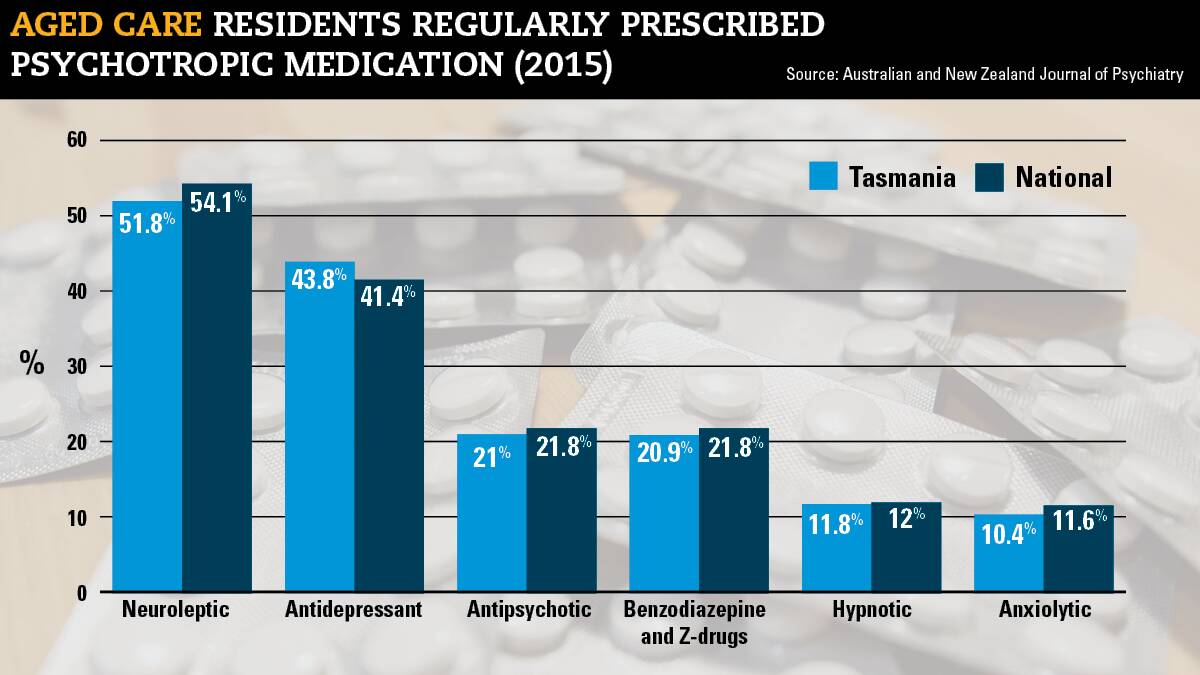
A Wicking Institute expert in reducing chemical restraint in aged care homes fears that recommendations from the royal commission won't stop the use of other forms of sedating drugs.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Commissioners recommended that only a psychiatrist or geriatrician be allowed to initially prescribe anti-psychotic drugs for people in residential aged care with individual patients to be reviewed on an annual basis, when repeat prescriptions can be made by a GP.
At the moment, GPs can prescribe the drugs with reviews every two years.
Dr Juanita Breen, a senior lecturer in dementia studies at the University of Tasmania's Wicking Institute, said her research indicated that once the use of one type of medication was restricted - such as anti-psychotics - another form of sedation would become prevalent.
She said the changes would be particularly difficult to apply in regional areas where there was limited access to psychiatrists and geriatricians.
"The problem isn't solely the GPs, because that's what it seems like it's implying, but you need to train the staff and give them support so they can apply these strategies and have time for proper assessments, and have enough staff to take someone away if they're agitated or upset," Dr Breen said.
"We'll just end up seeing the use of other medications go up. We're already hearing this is happening. People are looking for other things, opioid patches for example, they have a sedating effect.
"We're not the only country that has this problem. It has been shown in the US with their multi-million dollar program to reduce anti-psychotics, then everything else increased."
IN OTHER NEWS:
She said the students she encountered had a genuine willingness to receive the best training and avoid over-medication, but staffing pressures in aged care homes meant easy answers were often sought for complex behaviour displayed by residents.
Commissioners also called for greater education and training programs with consistency across the country.
"Numbers of care staff employed in residential aged care will have to be increased to ensure more time for better management of behavioural and psychological symptoms of dementia," the final report reads.
Following the 2019 case of Terry Reeves, who was given copious amounts of anti-psychotic drugs without his family's consent and ultimately died, the Australian Government brought in legislation requiring doctors to tell families if the drugs had been administered.
The legislation was widely criticised for being rushed and for failing to adequately protect those in aged care from inappropriate prescriptions.
Dr Breen said it was encouraging to hear there were plans for a complete overhaul of the Aged Care Act.


