In the late 1990s, a researcher in NSW first revealed the sheer scale of psychotropic drug use in aged care facilities.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
It prompted a parliamentary inquiry, and soon after, the issue became global. Australia was not alone with this problem.
But once the dust had settled, it faded into the background. The practice of immediate prescribing of psychotropic drugs for complex behavioural issues in aged care remained commonplace across Australia.
Dr Juanita Breen was working as a pharmacist when she became "puzzled" by the amount of sedating medications being used in aged care facilities. It sparked an interest that led her to becoming one of Australia's leading researchers into sedatives in aged care with the University of Tasmania's Wicking Dementia Centre.
Her research was highly cited in the aged care royal commission's interim report - an opportunity, Dr Breen said, to bring renewed long-term focus on the issue.
"After you have focused attention, what happens is that one or two agents are highlighted and use might go down a bit, but then there's an increase in other medications that do the same sort of thing," she said.
Dr Breen hopes that, this time, meaningful change can occur.
Why over-prescribing occurs
During her research involving 150 aged care facilities, one thing quickly became apparent - the levels of psychotropic medication had more to do with the facilities than the needs of the residents.
"Some homes do it with minimal medication, and some do it with a lot of medication," Dr Breen said.
"You have to ask, what's happening with the training, what's happening with the overall attitude of the leadership, what's happening with staff on the ground?
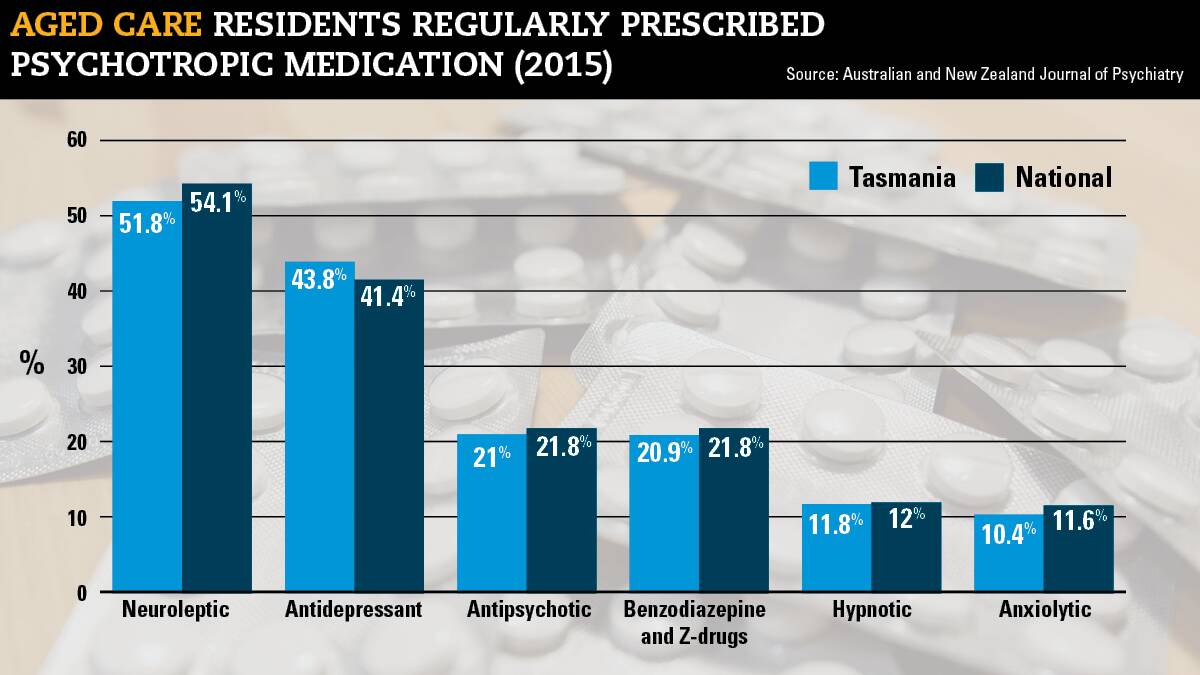
"Some homes didn't start a single drug, and others had 20 to 30 of their residents on them - as soon as they got into the home, they started on it. It made me think: it's not about the person or the type of people they have in the home. It's something to do with the culture: 'this is the way we're going to manage it'."
While "a small proportion of people" in aged care were suffering severe forms of dementia causing strong delusions or irrational beliefs, the vast majority were being prescribed psychotropic medication for agitated behaviour that pointed to other health conditions. Others had not even been diagnosed with dementia at all.
"There are things you should really be doing first to work out what's causing aggression to rule out other medical problems," Dr Breen said.
IN OTHER NEWS:
"The cause of the aggression could be the environment, they could be bored, or sometimes it can be that there's too much stimulus for someone used to a quiet life - that can be aggravating. They could just have a urinary tract infection that is causing them to call out and wander around.
"But instead of finding that out, it's just easier to give a pill. These medications in smaller doses will make people sedated, they'll stay in their beds, they won't be agitated."
The problem however, Dr Breen says, is that the types of medications - such as benzodiazepine and quetiapine - are used to treat conditions such as schizophrenia. They can have damaging side effects.
"Staff often don't know about the side effects. They didn't know it can cause strokes. They didn't know these medications cause falls. They think that, because these things happen to older people anyway, they didn't link it with the medication," Dr Breen said.
How to bring down usage
The royal commission has heard horrific stories of neglect from across Australia, including Tasmania.
And when it came to psychotropic prescribing - or "chemical restraint" - common problems were a lack of consent from families and guardians, the presumption of prescribing and low levels of staff training due to workforce issues.
In an attempt to address shortcoming, the RedUse system was trialled in Australia, led by Dr Breen and starting with 25 Tasmanian aged care homes.
It included an audit of drug use for residents with benchmarking. Training sessions were then provided in assessing residents' conditions and the side effects of certain drugs.
The main component involved a "champion" nurse who would recommend residents identified as benefiting from a reduction in psychotropic drug use. The nurse would liaise with the pharmacist to make recommendations to the GP.

The process would be reviewed and repeated every three months.
Dr Breen said they had excellent results.
"Because of the success of the initial Tasmanian trial, it was expanded nationally. Use had really gone down, so it was repeated again in 2016," she said.
"I can say that about 90 per cent of our homes experienced a reduction in the use of these types of medication.
"There is this real need for education. It's not as if the industry doesn't want it. When people were involved in this project, they were mostly really enthused. They wanted to have results, they wanted to do the best for their residents."
Where next from royal commission?
As the aged care royal commission prepares its final report, it has already foreshadowed several recommendations in regards to chemical restraint.
One involves using the Pharmaceutical Benefits Scheme to discourage "inappropriate prescribing".
"Given what we have learned about the frequent prescription of these types of medications by general practitioners, it may be appropriate to limit their initiation in residential aged care facilities to registered psychiatrists," the interim report states.
When chemical restraint has received widespread attention in the past, it usually results in short-term changes. Restricting the use of risperidone resulted in increased use of a similar alternative, quetiapine.
"It's just using an agent that is very similar, but isn't under the same prescribing restrictions. That's the issue, because ideally you want people to use non-medication options first," Dr Breen said.
And Tasmania could have a leading role to play, as home to the nation-leading Wicking Dementia Institute. Having access to this training has already resulted in the state having slightly lower rates of psychotropic prescription in aged care facilities.
Dr Breen said there was one critical factor that should guide all decision-making: the human rights of the residents themselves.
"You would regularly hear stories of people waking up, of relatives saying that they spoke to someone for the first time in a long time, they felt they were more engaged, they were able to do more things, they were able to talk, they weren't just sleeping all day," Dr Breen said.
"There are real tangible benefits. When you hear stories like that, it's really affirming."
The aged care royal commission is due to release its final report by the end of February.


