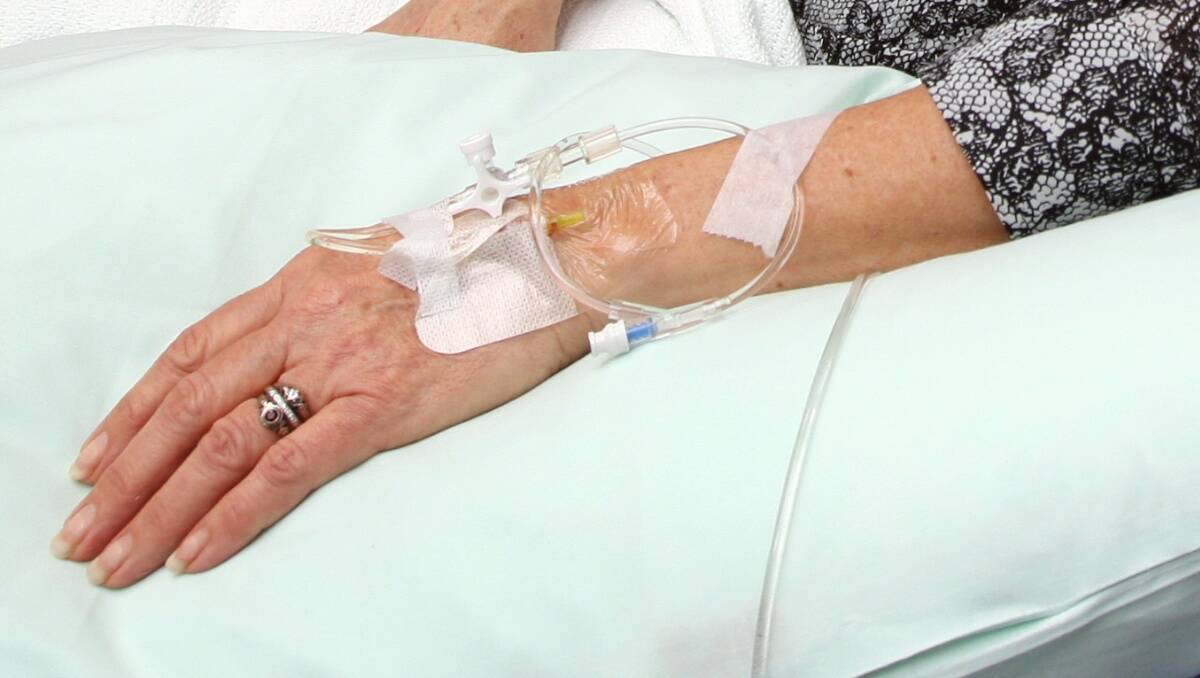
Amputation. Blindness. Kidney disease. Depression. Stroke.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
The staff at the John Morris Diabetes Centre know all too well the complications of diabetes.
But they say that as the prevalence rises and GPs are pushed to become experts on the chronic condition, health outcomes are improving. JODIE STEPHENS reports . . .
TWENTY years ago, while training at a hospital in Edinburgh, Anne Corbould saw about five pregnant women with gestational diabetes each year.
Now, as an endocrinologist at the John Morris Diabetes Centre attached to Launceston General Hospital, Dr Corbould sees between 100 and 150.
Dr Corbould, who works one week in Launceston and three in Melbourne each month, said the rise of gestational diabetes cases was one of the biggest changes she had seen in her career.
At the John Morris Diabetes Centre, Dr Corbould works alongside nurse educators, dieticians, podiatrists and psychologists to support patients with type1 diabetes and complex cases of type2 diabetes.
She said the centre had seen a rise in the complex cases, with complications including vision impairment, kidney disease, nerve damage and gangrene.
"It's because there is a lot more diabetes and because people are living longer with their diabetes," she said.
"About 30, 40 years ago, people died relatively young in a lot of cases because they had a heart attack, or stroke, or kidney failure, but these days we can prevent all those things."
Dr Corbould said this also meant centre staff couldn't see as many patients as the wanted, and the workload was "way more than we can cope with".
"The flip side of this is that the local GPs of Launceston, out of necessity and also their own interests, have become very expert in diabetes and the standard of care is very high," Dr Corbould said.
She said the long-awaited appointment of a full-time endocrinologist this year would help ease the burden on centre staff, and help them address service gaps.
Senior podiatrist Joe Rogers said the increased prevalence of diabetes was "half the attraction of the job, and half the depressing part of the job".
As the centre's senior podiatrist, Dr Rogers tackles complications caused by nerve damage to the feet and poor circulation, working with the team to try to prevent amputation.
"We do a lot of scaremongering around below-the-knee amputation, or large amputations, but they're less common," Dr Rogers said.
"Toe amputations, however, are really common."
Dr Rogers said nerve damage caused numbness in the feet, which meant patients couldn't feel when they had an ulcer.
He said this made it harder to convince them they needed to stay off their feet.
"People want time frames, they want to know that if they take a couple of weeks' sick leave, you will have it sorted," Dr Rogers said.
"You have to tell them, `this is diabetes foot, and we might be looking at four, six, eight weeks, even 12 months - it really depends'.
"And that's just for foot ulceration. Sometimes there are conditions within diabetes where bones and the architecture of your foot can actually collapse."
Dr Rogers said he was encouraged that GPs and the general public were increasingly aware of the centre's work - meaning better outcomes for patients.
"They're getting a better awareness - and we have got a way to go - that the work we're doing with diabetes is important and it's useful to them," he said.
"And that's not just for podiatry, it's across the broad spectrum of the diabetes centre."
As one of the centre's nurse educators, Sam Beattie helps people with diabetes who had been admitted to LGH, and supports people with diabetes to adjust to life with the condition.
Ms Beattie said in the hospital she saw people on life support with poorly managed diabetes, newly diagnosed diabetes, and patients going in for surgery or childbirth who need to avoid diabetes-related complications.
She said she didn't know what the future would hold for the newly diagnosed, as the people she saw in hospital were "the roll-on from 30, 40 years ago".
"So the people we're starting to work with now, by the time they're the age where they're in acute care with these kinds of complications, their picture might be very different," she said.
"But as for the tsunami of diabetes complications that the government's talking about, that any non-government organisation is talking about, I think we are going to see that.
"You can't argue with those statistics."
Dr Corbould said there was reason for optimism, with the rise of diabetes accompanied by improvements in treatments and insulins.
"Now, the outlook for people with diabetes is in fact very good and improving all the time," Dr Corbould said.
She said the centre was also having a significant impact through its support and programs - including a weekly clinic at LGH helping the increasing number of women with gestational diabetes.
"Since we started this clinic in 2006, the amount of babies that are large or need to go to the nursery because they've got low blood sugars or are unwell has really gone down dramatically," Dr Corbould said.
"So even though there's been more gestational diabetes, the babies are healthier because we are really controlling the diabetes very carefully."