Grave concerns have emerged over how Tasmania is placed to cope with the eventuality of borders reopening when COVID-19 vaccination rates across the country reach 70 to 80 per cent.
Subscribe now for unlimited access.
or signup to continue reading
Health groups the Australian Medical Association and the Australian Nursing and Midwifery Federation expressed their concern that an over-reliance on a National Plan for COVID-19 could see an already under-the-pump state health system left decimated.
National Cabinet last week went into detail about the availability of ventilators and intensive care unit capacity throughout Australia.
Prime Minister Scott Morrison said, following the meeting, more work would be done on assessing health system capacities around the country.
He said the work would target the "health and hospital system capacity and workforce needs to address expected demands under the National Plan".
The National Plan was based on much-lauded Doherty Institute modelling which has stated the country can begin to return to a COVID-normal with country-wide vaccination rates of 70 to 80 per cent.

In essence, as has been widely discussed in the national sphere, vaccination rates would prove to slow the transmission of the virus, but would not immediately stop it altogether.
Mr Morrison was confident it was the way for Australia to move forward.
"We must adjust our mindset. Cases will not be the issue once we get above 70 per cent. Dealing with serious illness, hospitalisation, ICU capabilities, our ability to respond in those circumstances - that will be our goal," he said.
The Doherty Institute's report outlined how more work needed to be done to transfer its projections across state borders. As it drew conclusions from particular populations, it freely conceded change in the projections would occur in differing regions.
"We will consider the way in which state-based differences may require tailored adaptation of the national strategy," it said.

Speaking to media in the wake of the latest National Cabinet meeting Premier Peter Gutwein remained defiant in the face of the National Plan.
"I will never cede away the state's responsibility to act should we need to act," he said.
The Premier's reluctance to entirely endorse the National Plan was echoed by the AMA and the ANMF, who said Tasmania's health system was not relevant to the plan's modelling.
The Tasmanian health system's nuance was made evident by the modelling, and the latest state government dashboard data on elective surgery waitlists.
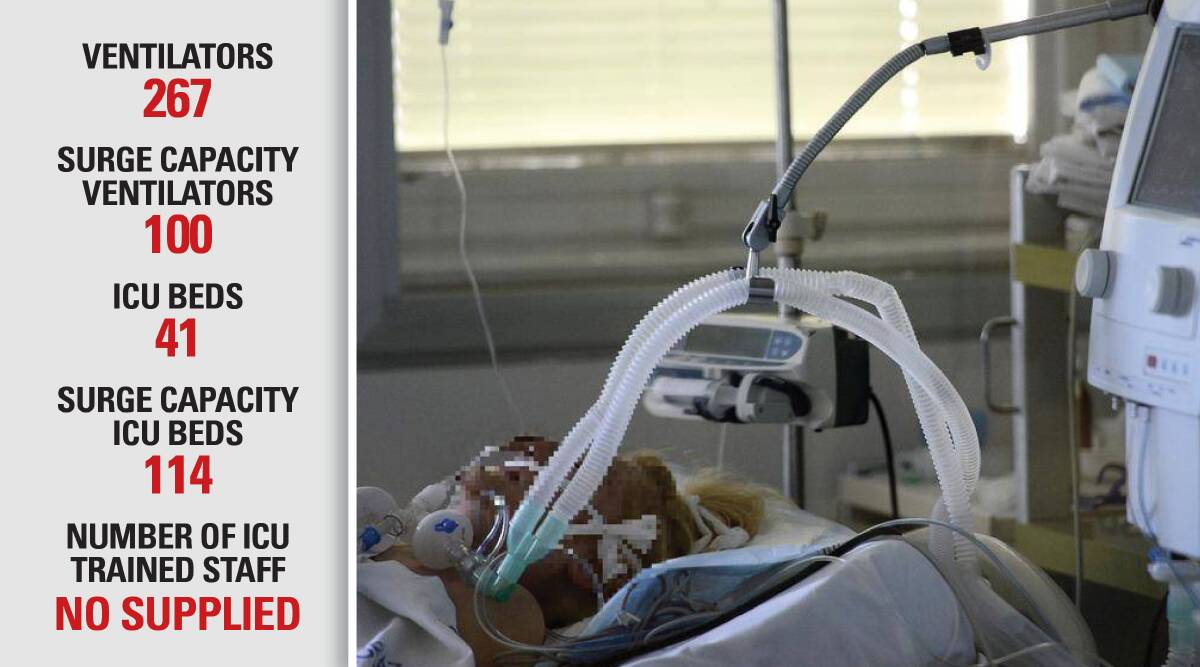
The modelling revealed across the state there were 41 Intensive Care Unit beds, while dashboard data showed 11,007 patients waiting for surgery and 1033 of them classified as needing surgery within 30 days.

AMA Tasmanian spokeswoman Dr Annette Barratt said the organisation was worried about how the state would cope with Delta COVID-19 cases indicated by the modelling, when considering the situation it was already in.
"The government has announced plans to cope with the inevitable Delta case in Tasmania, but we are concerned that our already stretched and exhausted health system may not be able to cope," she said.
"Tasmania needs to continue to do what is best for Tasmania, regardless of National Cabinet.
"The opening of our borders will need to be staged in such a way as to minimise the risk while continuing to have plans in place to prevent state-wide transmission. Uncontrolled outbreaks ... pose a major threat."

Similarly, Australian Nursing and Midwifery Federation Tasmania secretary Emily Shepherd said in a federal meeting last week fears were expressed about the federal government's reliance on the modelling.
"If we're suggesting we reach 80 per cent, we are accepting that 20 per cent of Tasmania's population could contract COVID-19, are we absolutely positive the health system is going to be able to respond? Realistically, the answer to that is no," she said.
The modelling was first initiated prior to the now developed understanding of the Delta variant of COVID-19, and Ms Shepherd said it was increasingly being acknowledged vaccination booster shots would be needed as a result of the virulence of the new strain.
"If we reach 70 and 80 per cent, is that the time we then need to consider booster shots? And are we operating under a false sense of security?" she said.
The concerns of both the AMA and ANMF carried through to the capacity of the Tasmanian health system to respond specifically to COVID-19 - with ventilators, ICU surge capacity and staffing expertise.
Information from the state government showed there were 267 ventilators currently in the state, with 100 more set to arrive, supplied by the federal government.
Dr Barratt questioned whether the surge planning in place - a potential 367 ventilators and 114 ICU beds - in Tasmania would be able to cope with an outbreak.
"We have sufficient ventilators, but insufficient staff trained to man them without putting other areas at risk if the outbreak was state-wide," she said.
Ms Shepherd said recently up-skilled workers operating without on the ground experience would add to current staffing shortages, meaning patients would need to prioritised and care outside of COVID-19 wards would likely be compromised.
A Tasmanian government health spokesperson said across the Tasmanian Critical Care Network there was confidence the state could respond to a potential surge in virus cases if required.
"There are several strategies in place to increase ICU capacity state-wide quickly if the need arises," they said.
"Through redeployment of ICU trained staff, we are confident staffing levels would be appropriate in the case of a surge."
The spokesperson was asked how many ICU trained nurses were enlisted in the Tasmanian Health Service, but they did not answer.
What do you think? Send us a letter to the editor:















