
It's been more than three years since Calvary Healthcare first put an unsolicited bid for a co-located private hospital in Launceston to the state government. However, there is still little to no new public information about what the proposal looks like.
Subscribe now for unlimited access.
or signup to continue reading
Rather, the $100 million bid remains in stage two of the assessment process with the Office of the Coordinator General, who is continuing to work through the proposal alongside Calvary and the Health Department.
At the same time, Tasmania's public health system remains strained. Elective surgery wait lists are at an all time high, while report after report continue to paint a damning picture of a health system and its public hospitals struggling to keep up.
Since it was first submitted, the opportunity for a co-located hospital in Launceston has been recognised as a "once in 100-year" opportunity to fundamentally change the way hospital and health services are delivered in Northern Tasmania. This includes providing different models of care that's accessible and affordable for both public and private patients.
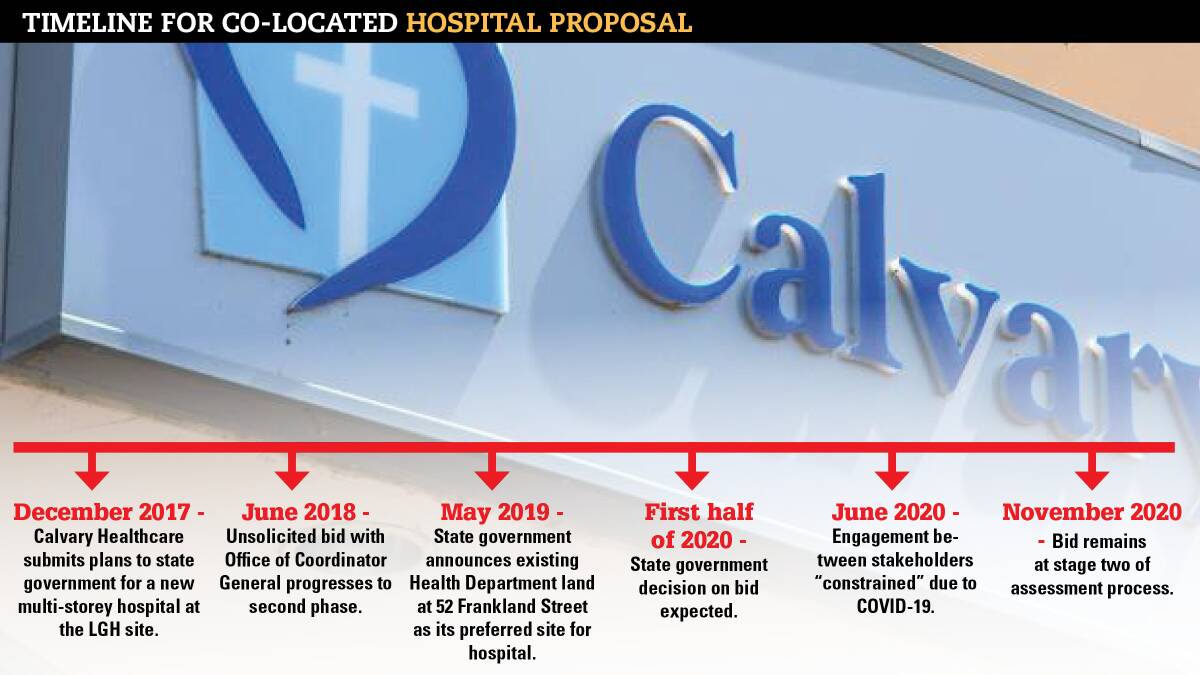
Prior to COVID-19, the government said it would make a final decision on Calvary's bid by mid-2020. It was also recognised as a key component to be considered within the broader Launceston General Hospital masterplan, also due to be completed in May 2020. Now, stakeholders are taking matters into their own hands.
In December, StLukesHealth reached out to members through an online survey to gauge their expectations of what a co-located hospital in Launceston could look like, and how it could help address existing shortfalls between the public and private systems.
With more than 1300 responses, members also shared their personal experiences, including challenges associated with a lack of specialists and outdated facilities. Over the next six weeks The Examiner will explore these issues and what the future of health service delivery in Northern Tasmania looks like.

Survey results:
When asked if they believed it was important for a new private hospital and the Launceston General Hospital to closely co-operate and share resources, 92.22 per cent of participants agreed.
A majority (76.2 per cent) also agreed that a new private co-located hospital should offer its own emergency department. This sentiment also came through strongly when respondents were asked to share their experiences with the existing system.
There was also considerable frustration among responders regarding the out of pocket costs for accessing care, when they already pay for private health. When asked if respondents believed that a new private co-located hospital would enable the North to attract and retain more specialists, 91 per cent agreed.
When asked to select the five most important services (from a pre-determined list) to include as part of a new private co-located hospital, the most popular choices were: elective surgery (90.44 per cent); private emergency department (71.08 per cent); palliative care (70.48 per cent); chronic pain unit (65.59 per cent); and acute hospital and psychiatric services (46.16 per cent).
The five most popular choices for the most important specialities were: bone and joint surgery (66.42 per cent); cardiac surgery (60.32 per cent); colonoscopy and gastroscopy (47.21per cent); cardiology (42.39 per cent); and back and spine surgery (40.36 per cent).
When asked about the biggest barriers to accessing services: 38.93 per cent said the specialist they need to see does not have a consultation clinic in the North; 27.26 per cent said that the service they need is not offered in the North; 21.01 per cent said the specialist they need to see does not perform surgery in the North; and 12.08 per cent said the service they need is not offered in the state.
When asked about what frustrates them most about accessing private hospital services in the North, 80 per cent of respondents noted the lack of a private ED, extensive waiting times, costs, parking, travel times from regional areas, lack of specialists, not enough staff, outdated facilities, lack of 24/7 access, the religious nature of private hospitals and the lack of maternity services as key issues.

Stakeholders have their say:
StLukesHealth chief executive Paul Lupo said the survey showed a co-located hospital was strongly supported by a community frustrated with a lack of specialists and up-to-date services.
"With a population that is ageing faster than other states and with high rates of chronic illness we really need to be at the forefront of how we will deliver health going forward so that the next generation does not experience the same ailments that are present now," he said.
"We see huge potential in this project and not just for those who have health insurance. We would like to see the wider community leverage off the great outcomes this project could deliver with attracting and retaining specialists to Northern Tasmania as well as the potential to improve patient care and outcomes. We need to challenge our current status quo on health."
Mr Lupo said it was important for the community to be consulted on the project as it reaches the critical stage - "we only have one shot to get it right".

A spokesperson for the Office of the Coordinator-General said the state government and Calvary were continuing to progress the unsolicited bid and were "actively working through stage two of the process".
"Probity advice has been sought from the outset to ensure the integrity of the decision making process is upheld and as specified in the guidelines - this is standard practice for the government for significant projects," they said.
"Stakeholder consultation has been undertaken with key groups from the health sector including representatives across a range of medical specialities, key hospital and health personnel, the medical training and research sector and medical related industries.
"If the proposal proceeds through final approval to contract and development [stage three) we expect that details would be publicly released well prior to construction as normal statutory approvals processes will apply."
Calvary Launceston general manager Grant Musgrave said it was committed to and respected the process underway, and was working with the government on progressing timelines.
"At this stage of the process we have consulted internally with relevant stakeholders and are working proactively with government to support the community into the future," he said.
"Calvary acknowledges the enthusiasm of the community and are confident that over time, with respect for the process, we will be able to achieve the best possible outcomes for the Launceston community."
Health Minister Sarah Courtney said a development of this size had "a range of complexities which take time to work through to ensure that the best possible health care outcomes are achieved for the state".
What do you think? Send us a letter to the editor:














