
Tasmania's major hospitals have moved beyond a crisis and into disaster, according to doctors, who say if a COVID outbreak or severe flu season hit the state now - the health system wouldn't cope.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
On Friday the Australian Medical Association and Australian Nursing and Midwifery Federation called for an urgent roundtable with clinical leaders, senior management and government to find solutions to pressures facing both the Launceston General and Royal Hobart hospitals.
AMA Tasmania spokesman Dr Frank Nicklason said both hospitals were at breaking point with ramped ambulances and patients left in waiting rooms because EDs were bed-blocked with admitted patients.

He said patients were also have critical elective surgeries cancelled amid bed block in the ICU, while acute patients were receiving treatment in recovery wards.
"It's almost a cliché, but it's a crisis situation that demands an urgent response. We need to see action on in the next week or so," he said.
"We've had the worst situation in our emergency department this week, we've had probably ever."
In a statement State Health Commander Kathrine Morgan-Wicks confirmed a meeting would be convened next week to discuss the issues.

"The Health Department always welcomes the input of the AMA and our clinicians, many of whom hold senior leadership positions within our hospitals and make decisions every day relating to our health system," she said.
"Demand issues are affecting hospitals around the country, particularly as all states, including Tasmania, continue to deal with the ongoing demands of COVID-19, in particular the vaccination task."
Dr Nicklason said pressure on both hospitals had been further complicated by the state's vaccination program, with several skilled nursing staff now working in COVID programs and quarantine hotels.
RELATED NEWS:
Amid Victoria's growing outbreak, he warned Tasmania could be facing its own disaster.
"We know we are dealing with a virus that's changed and is spreading more quickly and may be more serious," he said.
"We also have a flu season that may come upon us more quickly. We have a health system that is not coping at the moment, which would become completely dysfunctional if we got a wave of COVID or the ordinary flu season come into the hospitals."
However, Ms Morgan-Wicks said Tasmanians could have confidence that hospitals were preparing to implement winter bed strategies on top of ongoing initiatives being delivered under the statewide access and patient flow program.
"Spikes in demand, particularly for emergency department services, do occur and that is why hospitals implement escalation strategies," she said.
"Increasing demand pressures in a COVID-19 environment are being closely monitored and managed by all states and territories and information is being proactively shared."

Health Minister Jeremy Rockliff said he had met with the AMA and AMNF earlier this week to discuss how they could work together to improve access to care.
"It is in the best interest of patients and staff that we work together constructively to ensure we can get the right outcome," he said.
"I am absolutely committed to continue working with the AMA, ANMF and other stakeholder groups and have already made a commitment to meet regularly with the AMA."
Mr Rockliff said the AMA along with other stakeholders had been invited to form part of the government's new Health Staff Recruitment Taskforce.
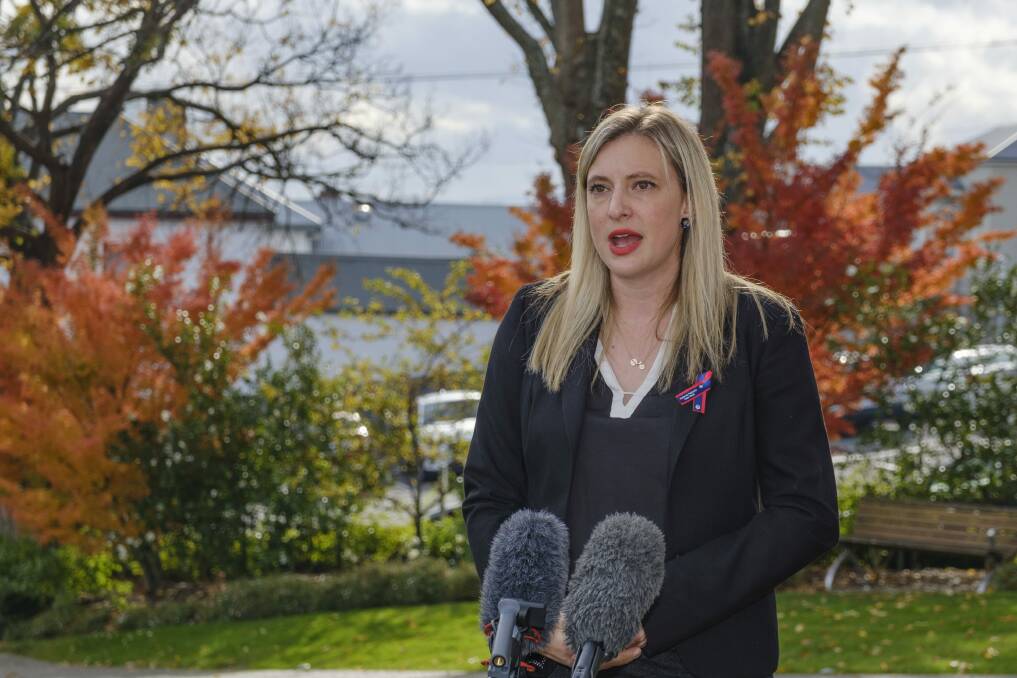
ANMF Tasmania branch secretary Emily Shepherd said the demand for critical care services across the state remained high.
"Our members and their colleagues are working incredibly hard. However, they cannot be expected to deliver the same level of service that has always been delivered without the needed services to do so safely, we will continue to advocate on our members behalf to ensure they are their patients are supported," she said.
"This is just another reminder how essential our skilled critical care nurse are and how important supporting the existing workforce while building this group of nurses is both now and for the future."

Access block has plagued Tasmania's major hospitals for a years, with a crisis health summit held in 2019 aimed at generating solutions.
Since then Dr Nicklason said there had been a shift of Commonwealth responsibilities onto the state's hospital system, with issues in the ED being compounded by aged and disability care patients with complex conditions, blocking acute care beds.
It's understood on Friday there were about 30 patients in each hospital waiting for care, requiring "sitters" to ensure their safety within the hospital environment.
What do you think? Send us a letter to the editor:
Our journalists work hard to provide local, up-to-date news to the community. This is how you can continue to access our trusted content:
- Bookmark www.examiner.com.au
- Make sure you are signed up for our breaking and regular headlines newsletters
- Follow us on Twitter: @examineronline
- Follow us on Instagram: @examineronline
- Follow us on Google News: The Examiner


