
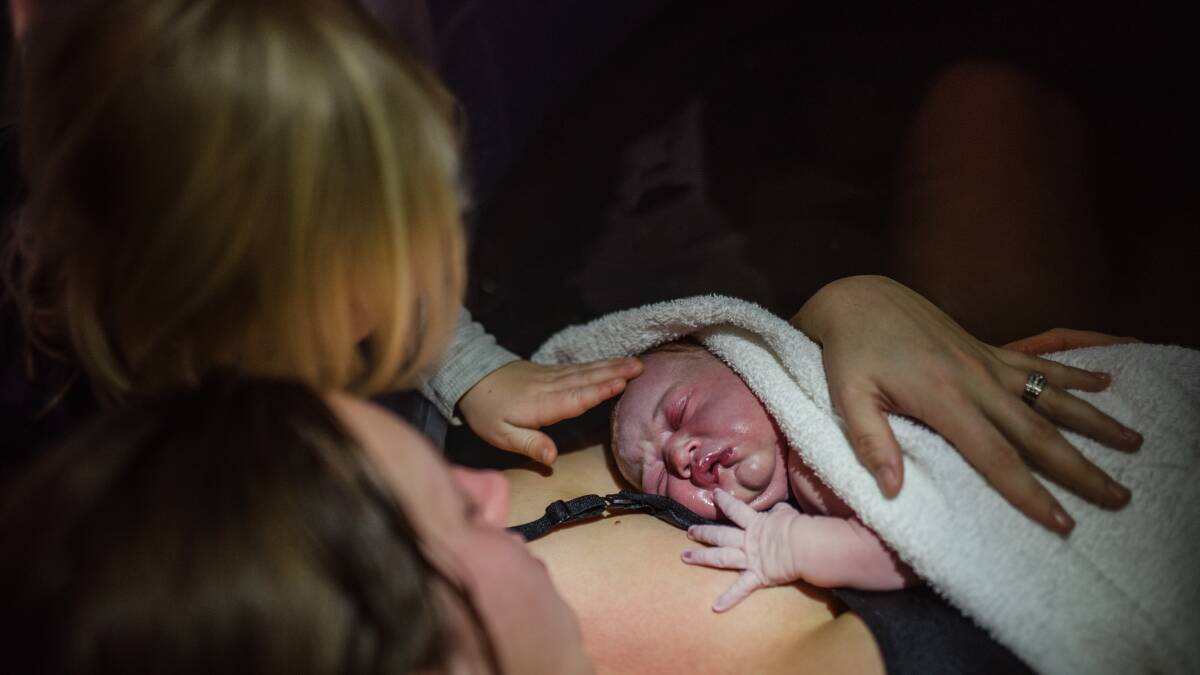
Tasmanian mothers are increasingly deciding to give birth at home after their negative and traumatic experiences of labouring and birthing on hospital maternity wards.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
A lack of support in maternity wards, and a lack of information provided to women about medical birthing processes and interventions before and during labour, which results in the giving of uninformed consent, are some of the reasons provided by two North-West mothers who chose homebirth for their second-born children.
Research shows that these negative birth experiences can contribute to the development of post-natal depression, and can also result in post-traumatic-stress-disorder (PTSD).
According to the Australasian Birth Trauma Association about 9,000 women each year develop PTSD after giving birth, but many go undiagnosed.
Countless others experience some form of birth trauma, which can relate to physical injury but also the lingering emotional and psychological impacts of a less-than satisfactory birthing experience.
For Bethany Ayton, 26, of Devonport, there were a range of issues within the hospital setting that resulted in her birth trauma, and which led her to seek a different option for the birth of her second child.
I felt like I didn't deliver my baby. He was pulled out of me, and that was quite traumatic. Even now it is still raw for me, five and a half years later.
- Mother of two Bethany Ayton.
For one, she wanted to have as natural birth as possible but felt unsupported by the hospital to fulfil these wishes.
Secondly, she said there was little birthing guidance from midwives during labour, where she experienced a lack of help from hospital midwives to find alternative birthing positions to move and deliver her difficulty positioned baby.
She believes this lack of assistance on the maternity ward contributed to the eventual vacuum-delivery of her son.
"The real lack of support is what got me. I felt so vulnerable but it just didn't seem to matter to any of them. I was a number and they just wanted to get my baby out," Mrs Ayton said.
"I was told they would need to assist delivery but I did not necessarily know what this meant," she said.
"All of these things just happen to you without you knowing, and you feel violated because you have no idea that they are doing these things to your body.
"Even after delivery, in regards to delivering the placenta, they said 'we've given you this drug' but I didn't know what they were giving me."
After the birth Mrs Ayton said she felt disappointed and confused, and has attended counselling to assist with these thoughts.
"I felt like I didn't deliver my baby. He was pulled out of me, and that was quite traumatic. Even now it is still raw for me, five and a half years later," she said.
"I thought that I had let my son down and I felt like I failed myself. I felt that I had done something wrong but I didn't know what that was. I also felt like the hospital had failed me."
Same medical approach regardless of healthy pregnancy or not
Looking back on her experience, Mrs Ayton questions why medicalised births and interventions become the norm for all women, including those who are young, and who experience a normal and healthy pregnancy.
"When I was labouring at home I was comfortable, I was at ease, my contractions were lovely, and regular, but as soon as I walked into that hospital setting it wasn't calming and it wasn't relaxing, it was clinical and it was medical," she said.
"Rather than medicalising every single birth that walks through the hospital door, including low risk, healthy and young women, whose babies are healthy, birthing should only become medicalised when it is necessary."
During her second labour for the birth of her daughter, a homebirth, she said her private midwives coaxed her through the labour, suggesting various positions to assist delivery of the baby who was also in a difficult position.
"After the birth of my daughter at home I felt empowered, I was on a complete high, climbing out of the birth pool, laughing, but at my son's birth the midwives just wanted to get my baby out, none of them truly cared about the person I was, or how I was feeling. You are just someone who is birthing a baby."
I may have given consent but it was not informed consent. There was no discussion around why we need to do this procedure or that.
- Mother of two Carol Steyn, of Ulverstone
North-West mother Carol Steyn, 35, of Ulverstone, said her experiences of birth within the hospital setting were equally disappointing.
She decided on homebirth to get consistent care with the same midwives, to regain control over her birthing experience, but also because of the very quick delivery of her first child.
Her main frustrations with the system occurred after the birth, and she raises issues of informed consent.
Mrs Steyn said after giving birth she did not get skin to skin contact with her baby, she required stitches that were given without pain relief, and she was given a suppository despite telling her doctor that she did not want one.
She said things were done to her without any explanations.
"I may have given consent but it was not informed consent. There was no discussion around why we need to do this procedure or that," Mrs Steyn said.
"The obstetrician ran out of numbing [treatment]. There were only six stitches left and they were done in cold blood. Then the catheter went in and I was given a suppository," she said.
"I would not usually choose to take medication and to then just have it rammed up my bum, I don't think that was appropriate.
"I left that experience and later, felt disappointed."
For the birth of her second child Mrs Steyn was adamant that she did not want to go through the public system again.
"I wanted it to be natural, I just wanted to do it my way. Private midwives were the only other way, and my private midwives were just beautiful. The care I received was just unbelievable."
Alternative birthing options are available, but women need to be proactive
The experiences of both Mrs Ayton and Mrs Steyn are familiar with Tasmanian doula Genevieve Sayers who has long-lobbied for maternity reform.
"Women choose homebirth because they get continuity of care from a known midwife, it does not involve going to the hospital and instead is in their home in their normal, safe and familiar environment, they can have who they want at the birth, and they have more control over what happens," she said.
"They look for something different because they weren't happy with their first experience, whether it was trauma, an intervention of some kind, or they just weren't happy with the care for some reason."
Mrs Sayers said general practitioners generally inform expectant mothers of just two options for giving birth; either in the public or private hospital system, and this is a major problem.
"Referrals depend on whether women have private health or not. That is not the best way to direct women into maternity care," Mrs Sayers said.
"It should be 'do you want a normal birth?' Here are some options with low interventions, rather than just directing them immediately into the hospital system," she said.
"Women don't realise there are options out there, and they don't get that information unless they really go looking for it.
"Most general practitioners are either unaware aware or are not trained to acknowledge or understand that there [birthing] options exist."
Mrs Sayers said hospital maternity care was not women-centered and instead was driven by budget-considerations.
"It means you put midwives on shifts, women lose continuity of care, they lose familiarity. It is about budgets and staffing and running a system, it becomes about money."
She said a general reliance and acceptance on the word of medical professionals, influenced by a social trend of simply accepting the word of medical experts and not asking questions, carried into the hospital setting.
"You always have a choice, and you always have the right to decline," she said.
"Just because something is a hospital policy or a recommendation, or they propose a certain intervention, doesn't mean it is the right choice for you."

Both North West mothers now have two beautiful and healthy children, and both delivered babies in the hospital and at home.
The experiences, they say, were vastly different.
Homebirth, for both of them, was the best choice.
Mrs Ayton added that she does not want to scare new mothers, and realises that homebirth is not for everyone.
Rather, she wants women to be aware of their options, and to make sure they have someone at the birth who knows what they want, who can be their spokesperson to vocalise those wishes.
"As a labouring mother you lose a bit of your cognitive decision making ability, so you need someone there who can stand up for you."
She said after the births, she joined a local Australian Breastfeeding Association group, and naturally, the women shared their birthing stories.
The experience, she said, was healing.
"It was quite helpful. We were all able to share our personal experiences and I discovered that a lot of the mums had stories similar to mine.
"It made me realise, why on earth is the system the way it is?
"If there are so many of us sitting here comparing stories which are so similar, there is something wrong."


