More than 2000 people work at the Launceston General Hospital in roles ranging from surgeons and nurses, to administration and cleaning.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
But when a patient requires surgery, there is one department in particular that serves as the basis for ensuring quality care - the sterilisation department.
Tucked away out of sight the work carried out in the SD is a vital cog in the hospital's wheel.
From the water used to clean equipment to the air in the department itself - everything is quality controlled.
And while most patients would be none the wiser about the types of instruments used on them during surgery or where they came from, for the SD team these elements are their bread and butter.
Consisting of about 17 operational staff, mainly SD technicians, an instrument tracking system's administrator and a nurse unit manager, the department's role is to ensure the availability of sterile and thermally disinfected items as needed.

As nurse unit manager John Taylor explained, the "organised chaos" of the SD department is a combination of strict standards, science and attention to detail.
"When it comes to surgery, the work we do here is paramount," he said.
"You can imagine microorganisms of any description on your instruments.
"Performing a surgery and then sewing a person up - it makes for a beautiful place for germs to incubate.
"The technology behind the steralising, while the science hasn't changed a lot, the technology behind that science certainly has changed a lot.
"Everything you see here is standards driven, down to the the final water that washes the instruments.
"Organised chaos is exactly how I would describe it.
"It peaks and drops, depending on how many theatres are running and what emergencies might come in.
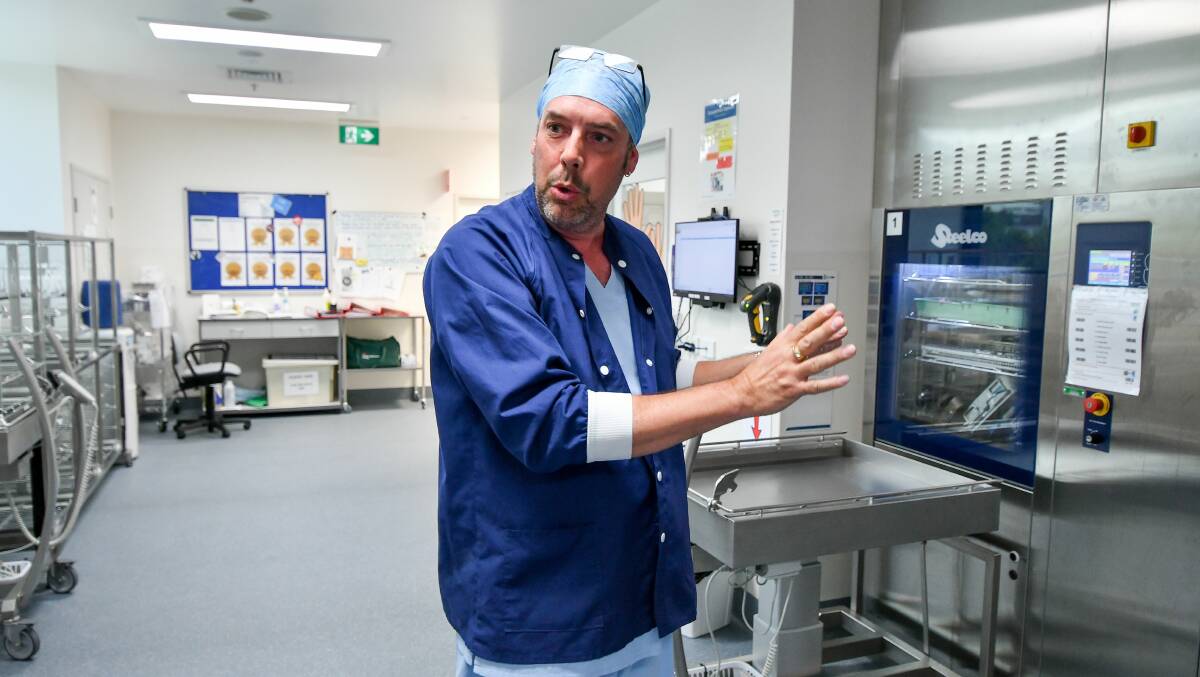
"But when it's up and running this place hums. The whole team is amazing."
The SD is responsible for the specialised cleaning, packaging and sterilisation of reusable medical devices, also known as RMD's.
When it comes this, they must conform to a strict set of national and international standards - something that is regularly audited.
Mr Taylor said the standards ensured a high level of quality care was maintained, even if the patients themselves weren't aware of everything that went into the process.
All soiled instruments go through a decontamination process, that washes the instruments resulting in thermal disinfection at 90 degrees.
Once cooled and dried, this allows staff to safely handle and inspect each and every instrument for functional and cleaning efficacy, prior to being sorted into their respective sets.

Instrument sterilisation is achieved by either steam or low temperature plasma hydrogen peroxide.
In the case of steam, the LGH has three large sterilisers that repeatedly pulls each load down into a vacuum, removing all air, before injecting steam and raising the vessel pressure to 220Kpa and 135 degrees.
The load is held at this temperature for five minutes which is enough to destroy all living organisms.
As Mr Taylor put it, this process and only this process ensured that ever single instrument was made sterile.
"That science is what kills every live organism. That's what we call sterile," he said.
"And technology has allowed us to make great advancements in this.
"Back in the day, these sterilisers would have had one boiler supplying steam to all three, but it would have struggled to make enough steam.
"Plus, everyone used tap water, which then had to be treated with chemicals by the engineering people in order to get the quality of water needed to make steam.
"So we have removed all of these problems, just in technology upgrades."
For heat sensitive equipment a similar result is achieved using a plasma hydrogen peroxide steriliser, but with a maximum temperature of just 50 degrees.
On completion of each load, this machine leaves nothing but the sterilised equipment and water vapour.
All RMD's are processed using a packer and checker system, where two technicians are used per instrument set to ensure accurate instrument count and quality.
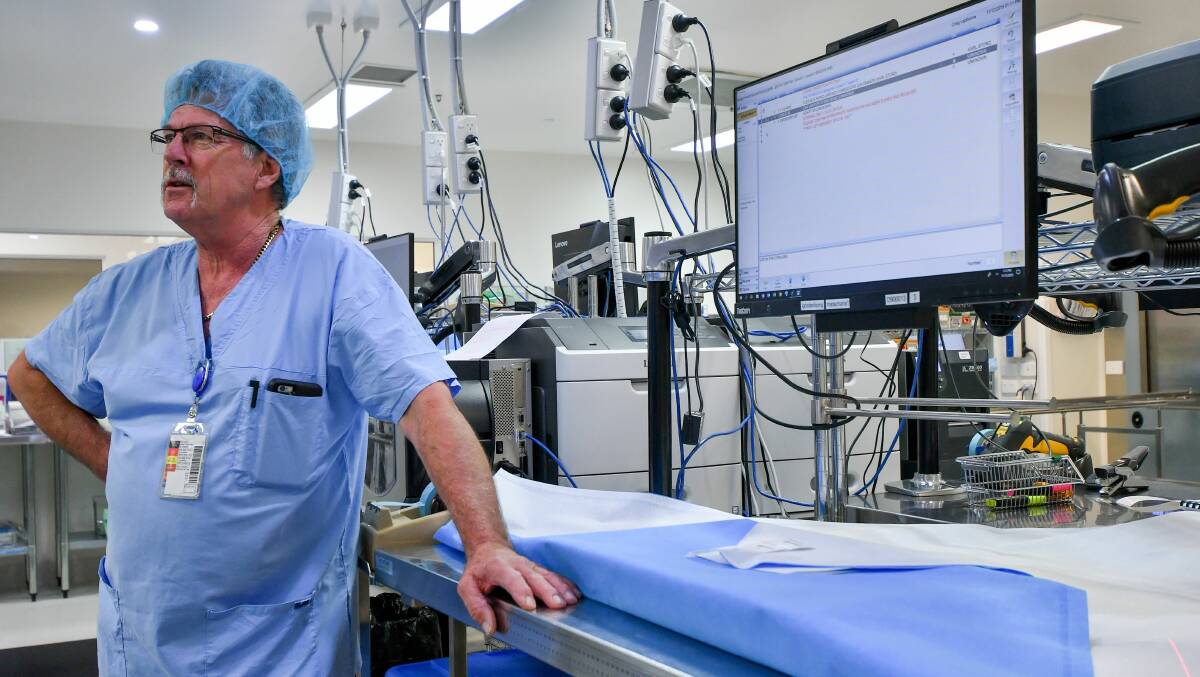
All surgical instruments are of the highest quality and are tracked using a state of the art instrument tracking system.
Staff scan and the system stores each set into their respective steriliser cycle in SD, recording both cycle parameters and load contents.
In the Operating Room Suite, nursing staff then scan instruments used during an operation, to the patient's file.
On return to the SD, used instruments are then scanned back in, ensuring full traceability.
On any given day the thousands of pieces of surgical equipment would come through the steralisation department.
For every operation that goes on in surgery, there is a full set of instruments that need to be available - in some cases multiple cases.
But for most of the staff, identifying each one and what they're used for becomes just another part of the job.
For steralisation technician Craig Lapthorne, who has worked at the LGH since 1984, his role in the SD has kept him on his toes.
"It's just really, really interesting work," he said.
"You have all the instruments.
"You are learning something every day and any day is different."
"Patients don't know.
"They wouldn't have a clue of all that's involved down here.
"So it can be very interesting to see what instruments are used for each operation.
"There's thousands of instruments in the system and nearly every body in this department know what each one is, just by looking at it.
"That's part of the fun."


