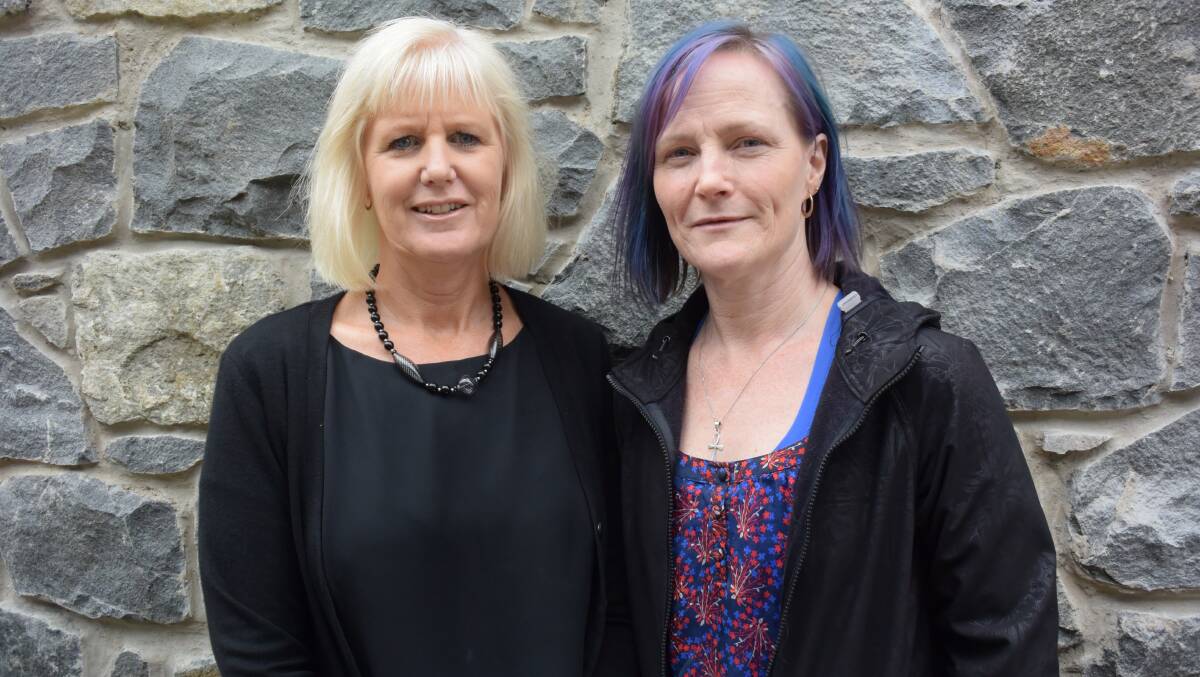
Amid concerns over the end of federally-funded palliative care programs, the state continues to provide end-of-life services for Tasmania.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Although some federally-funded services in palliative care are ending, Tasmanian Health Service providers have stressed that palliative care is available.
THS primary health North area manager Fiona Young and Specialist Palliative Care Service nurse unit manager Kristen Aylmer said there was “much confusion and concern” among the public regarding palliative care in the state.
For patients with life-limiting illness, a significant portion of the care usually takes place at home.
It can be provided by a network of carers, family and health professionals.
I am concerned that the discussion around the end of funding to Palliative Care Tasmania has led a number of people to incorrectly think that state government services to palliative patients has been reduced.
- Health Minister Michael Ferguson
The THS Specialist Palliative Care Service provides clinical leadership and delivers professional advice in palliative care practice across that state. The service has multi-disciplinary teams in the North, North-West and South.
The Northern team of the service consists of specialist medical, nursing and allied health, including occupational therapists, social workers and volunteers.
The team supports clients and their families and carers across all settings including at home, residential aged care facilities and rural health care facilities, many of which have dedicated palliative care beds.
It also provides medical and nursing liaison to the LGH and private hospitals, giving advice on symptom management and discharge planning.
Volunteers participate in support programs, including Walking Through Grief.
The program facilitates a walking group for people dealing with the loss of a loved one to life-limiting illness, and forges friendships and offers emotional support.
Volunteers with the Specialist Palliative Care Service also provide dying Tasmanians with practical support and a friendly face to chat with.
Confusion was caused by the end of some federally funded services, Ms Young and Ms Aylmer said.
The Better Access to Palliative Care program, a one-off assistance package, was funded under the Tasmanian Health Assistance Package by the federal government.
The palliative care program began in June 2012 and was due to finish in June 2016. The program provided $49.2 million over four years for palliative care services.
It provided funding to services including the District Nurses of Tasmania to facilitate hospice@HOME, and Palliative Care Tasmania.
The contracts for PCT and the District Nurses for hospice@HOME were extended in April 2016.
PCT’s funding ended in September 2016, but the organisation worked on short-term projects.
PCT provided community education to Tasmanians about end-of-life care.
The service, which gradually ended staff contracts, was due to completely end last week.
But it was thrown a lifeline by its council, which will use reserve funding to keep the PCT Hobart office open at least one day a week until mid-2016. PCT general manager Colleen Johnstone will continue to staff the office.
The service will wait for the state budget to inform its future. Its Launceston and Devonport offices were closed.
Hospice@HOME will stop accepting referrals after March 31, and funding ends in June. The District Nurses reassured current clients of the program that their services would not be ceased.
The District Nurses chief executive Kim Macgowan said the news about PCT had caused confusion among clients who received hospice@HOME services.
She said all clients who are in the hospice@HOME program at the end of June would continue to be supported with in-home care until they no longer required services.
Health Minister Michael Ferguson said he was “concerned that the discussion around the end of funding to Palliative Care Tasmania has led a number of people to incorrectly think that state government services to palliative patients has been reduced.”
“There has been no reduction or cuts to state-funded palliative care services,” Mr Ferguson said.
“The government has made strong representations to the federal government regarding the Better Access to Palliative Care funding,”he said.
“We are working constructively with PCT and actively investigating opportunities to support them.”
The THS has a contract with Calvary Health Care Tasmania for a minimum of four public beds in the Melwood Unit at St Luke’s in Launceston.
The THS is flexible with the arrangement and pay for additional public beds for palliative care patients as necessary. The Specialist Palliative Care Service also admits private patients.
Melwood is a 15 bed unit which with experienced palliative care staff which provides a peaceful environment facilitating symptom management and end of life care.
“The idea is everything that we [SPCS] do … is to provide support to maintain people’s quality of life and their independence as much as possible in line with their priorities,” Ms Aylmer said.
“It is absolutely a privilege to look after people who have a great need.”


